|
Olaparib (brand name Lynparza) was approved for use in India as a treatment for certain types of cancer, particularly ovarian and breast cancer. However, it's important to note that new medications and alternatives can become available over time.
Olaparib is an anticancer medicine referred to as the Poly Adenosine Diphosphate-Ribose Polymerase (PARP) inhibitor. Olaparib Tablet has been developed as a maintenance therapy to treat adult patients with cancer in the ovaries, fallopian tube, peritoneum, pancreas, prostate due to BRCA mutation and have completely or partially responded to platinum-based chemotherapy. Olaparib Tablet is available in the doses of 100mg and 150mg and the strength varies according to the patient’s health condition. Olaparib brands in India If you are looking for information about Olaparib (Lynparza) in India, including alternatives or availability, I recommend checking MrMed website for low price substitutes. Lynparza & Bracanat 2 brands are available in India. Lynparza Tablet: Lynparza 150mg Tablet is a targeted anticancer drug belonging to the category of PARP inhibitors. It specifically acts against ovarian cancer due to mutation in BRCA genes. Bracanat Tablet: Bracanat 150mg Tablet is usually indicated as maintenance therapy after a person completes a platinum-based chemotherapy regimen for ovarian cancer. Some of the common side effects of Olaparib Tablets are.
Cancer treatments, such as targeted therapies, chemotherapy, immunotherapy, and radiation therapy, are available to healthcare professionals in India. Because new drugs and treatment options are always being discovered and approved, it is critical to collaborate closely with your healthcare team to find the best treatment plan for your individual case. Furthermore, India's pharmaceutical sector is expanding, and generic versions of Olaparib or similar medications may be accessible at a reduced cost. Your healthcare practitioner can also advise you on these possibilities.
0 Comments
The blood malignancy known as chronic myeloid leukaemia (CML), also called chronic myelogenous leukaemia, primarily affects the bone marrow and blood cells. It belongs to the larger class of malignancies known as leukaemia, which includes those that start in the bone marrow and impact blood cell formation.
Granulocytes, which are abnormal white blood cells, grow and accumulate uncontrollably in the bone marrow and blood, which is a hallmark of CML. The usual equilibrium of blood cell types is upset by the overproduction of white blood cells, which can result in a variety of symptoms and consequences. The Philadelphia chromosome (Ph chromosome), a genetic anomaly, is frequently the underlying cause of CML. A new gene termed BCR-ABL1 is created when a portion of chromosome 9 fuses with a portion of chromosome 22, causing this genetic abnormality. This gene's mutation results in the production of the BCR-ABL1 tyrosine kinase protein, which is essential for the unchecked expansion of white blood cells. The signs and symptoms of CML might differ, and in the early stages, some people may not show any symptoms at all. Fatigue, weakness, weight loss, fever, night sweats, an enlarged spleen (splenomegaly), and stomach discomfort brought on by the enlarged spleen are some of the common symptoms. Tyrosine Kinase Inhibitors (TKIs): TKIs are the cornerstone of CML treatment. The active component of the Bonitar 400mg Tablet is bosutinib. It is a member of the class of drugs known as tyrosine kinase inhibitors. They work by blocking the activity of the BCR-ABL1 tyrosine kinase protein, thereby inhibiting the uncontrolled growth of abnormal white blood cells. Some of the commonly used TKIs for CML treatment include:
For people with CML, routine monitoring and follow-up are crucial to gauge therapy efficacy, control potential adverse effects, and guarantee early diagnosis of any alterations. With the development of targeted treatments, the prognosis for CML has substantially improved, and many people with CML can have relatively normal lives with the right medical care and therapy. However, depending on variables like the stage of the disease at diagnosis, how well a patient responds to treatment, and their own health situation, the management and outlook may differ. A popularly prescribed antiviral drug called valacyclovir is used to treat viral illnesses brought on by the herpes virus, such as genital herpes, cold sores, and shingles. It is a crucial tool for managing and containing outbreaks and alleviating the suffering of those afflicted. In this post, we'll look into valacyclovir's applications as well as any possible negative effects.
Uses of Valacyclovir:
How valacyclovir Works: Because valacyclovir is an antiviral drug, the body transforms it into acyclovir, which is its active form. Acyclovir prevents the herpes virus from replicating by decreasing the activity of the enzyme DNA polymerase. Valacyclovir aids in the management and control of epidemics by preventing the virus's ability to multiply, minimising its impact on those impacted. Potential Side Effects: Most people handle valacyclovir well and only experience minor side effects. Typical negative consequences could be:
It is important to remember that these side effects are typically moderate and transient and that not everyone will experience them. Before beginning Valacyclovir medication, any pre-existing medical disorders or allergies must be disclosed to your healthcare professional. Patients with immune system or kidney issues may need different dosages or more attention throughout treatment. A complete list of all the medications you are taking must be given to your healthcare provider because valacyclovir may interact with some drugs, such as probenecid and cimetidine. An effective antiviral drug for treating and controlling herpes infections is valacyclovir. Millions of people worldwide have found respite thanks to its ability to lessen the severity and duration of outbreaks. Even though side effects are frequently minor, it is crucial to be aware of them and to talk to your doctor about any worries. Valacyclovir can dramatically raise living standards for those with herpes infections when used as directed. The list of possible prostate cancer treatments includes surgery, radiation therapy, hormone therapy, chemotherapy, targeted therapy, and immunotherapy. Your treatment options will depend on several factors, including how fast the cancer is growing, whether it has spread, your general health, and any anticipated benefits or symptoms of prostate cancer treatment. A prescription medicine called Lynparza 150mg Tablet contains olaparib. It is used to treat ovarian, breast, pancreatic, and prostate cancers. Many medications used in prostate cancer treatment have alternatives of olaparib lynparza that offer similar benefits at a lower cost like Bracanat 150mg Tablet.
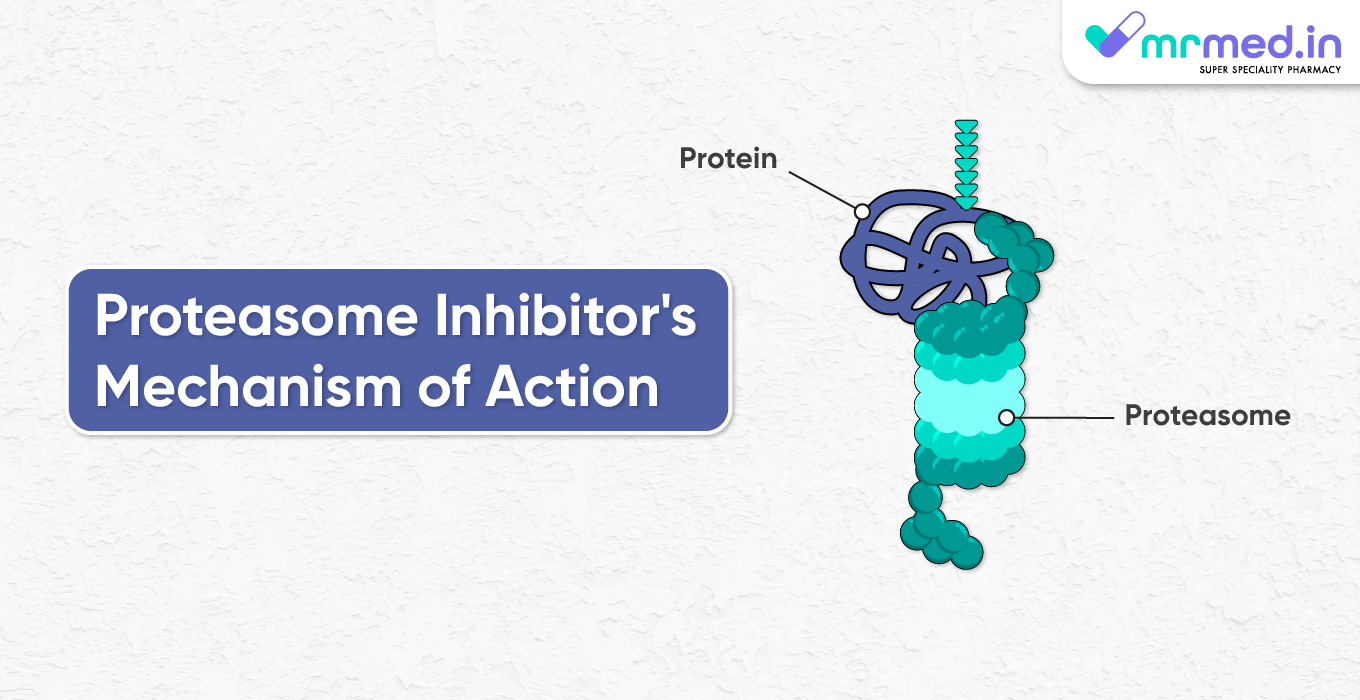
Prostate Cancer Symptoms Prostate cancer's early stages may not be accompanied by any obvious symptoms. However, if the cancer worsens, some symptoms could be: Urinary Symptoms: Painful urination, frequent urination (particularly at night), poor urine flow, frequent urination, and blood in the urine. Erectile Dysfunction: Inability to achieve or sustain an erection. Pain: Discomfort in the lower back, upper thighs, hips, or pelvic region. Prostate Cancer Diagnosis A variety of tests are commonly used to diagnose prostate cancer, and these tests may include: A doctor does a digital rectal examination (DRE) by inserting a gloved finger into the rectum and feeling the prostate for anomalies. Prostate-Specific Antigen (PSA) Test: A blood examination that gauges the prostate's protein PSA levels. PSA readings that are elevated may be a sign of prostate problems, including cancer. Biopsy: Prostate tissue samples may be collected during a biopsy to be analysed further if the PSA levels or DRE results are alarming. Conclusion For men over the age of 50, routine screenings, including PSA and DRE testing, are recommended. However, the decision to perform screening should be based on a thorough conversation with a medical professional, as the benefits and risks of each can vary.  A disorder known as immunoglobulin deficiency, often called antibody deficiency, is characterised by the immune system's failure to create enough immunoglobulins, also known as antibodies. The immune system produces immunoglobulins, vital proteins that protect the body from diseases brought on by bacteria, viruses, and other pathogens. Immunoglobulins come in various forms, including IgA, IgG, IgM, IgD, and IgE. Each kind contributes differently to the immunological response. These immunoglobulin deficiencies can increase vulnerability to infections and repeated illnesses. Immunoglobulin deficiency comes in a variety of forms, including: IgA deficit: The most prevalent kind of immunoglobulin insufficiency, IgA deficiency is characterised by low or nonexistent IgA antibody levels. It could raise the risk of gastrointestinal and respiratory infections. Low levels of IgG antibodies, which are essential for long-term immunity, characterise this kind of IgG insufficiency. Bacterial infections may be common in people with IgG deficiencies. Combination immunoglobulin deficiency causes a more severe and pervasive immunological dysfunction due to deficits in numerous immunoglobulins. The main goal of immunoglobulin replacement therapy, which treats immunoglobulin deficiency, is to restore any lacking or insufficient immunoglobulins. Concentrated immunoglobulins from healthy donors are infused into the patient to give this treatment. Subcutaneous injections or intravenous (IV) infusions are two ways to administer the medication. The goals of immunoglobulin replacement therapy are: Boost the immune system: By giving the body enough immunoglobulins, the therapy aids in enhancing resistance to infections. Immunoglobulin injections regularly can help patients live better lives by lowering the incidence and severity of infections. Passive immunity: The immunoglobulins offer instant defense against some illnesses, particularly in patients with compromised immune systems. The kind and severity of the immunoglobulin deficiency determine the frequency and dosage of immunoglobulin replacement treatment. Some patients could need infusions every few weeks, while others might require more frequent care. Bharglob Injection is an extract of human blood containing antibodies (own defensive substances of the body) to diseases, available as a solution for infusion. Individuals with immunoglobulin deficits must collaborate closely with their medical professionals to monitor their condition and modify treatment as necessary. In addition, successful management of immunoglobulin deficiency depends on preventive measures, including vaccines and preventing infection exposure. A class of medications known as proteasome inhibitors are used to treat cancer, particularly in treating certain blood malignancies, including multiple myeloma and mantle cell lymphoma. Proteasomes, a cellular component in charge of protein breakdown, are targeted, and proteasome inhibitors inhibit their activity as part of their mechanism of action.
The main job of the proteasome, a large protein complex located in the cytoplasm and nucleus of cells, is to break down unneeded or damaged proteins. This procedure is crucial for preserving cellular homeostasis, controlling protein levels, and getting rid of aberrant or misfolded proteins that might harm the cell. As a result of the proteasome's action being blocked by proteasome inhibitors, proteins that ought to be destroyed accumulate. As a result, several crucial cellular functions are interfered with, ultimately resulting in cancer cells dying. The following are the crucial phases in proteasome inhibitors' mode of action:
When the overall volume of blood circulating throughout the body significantly decreases, a condition known as blood volume loss, or hypovolemia occurs. Numerous things, such as bleeding, fluid loss, trauma, or specific medical disorders, might contribute to this syndrome. The symptoms and treatment may differ depending on the severity and underlying cause of blood volume loss.
Symptoms of Blood Volume Loss (Hypovolemia):
Treatment of Blood Volume Loss: Replacement of the lost fluid and therapy of the underlying cause is the main goals of treatment for blood volume loss. Following are some possible general actions: Replacement of fluids: Fluids are given intravenously (IV) to increase blood volume. The kind and quantity of fluid required will vary depending on the condition's severity, the reason for fluid loss, and the patient's requirements. Commonly used isotonic crystalloid solutions include lactated Ringer's solution and normal saline. Addressing the Underlying Cause: For hypovolemia to be effectively treated, the underlying cause must be found and addressed. Stopping bleeding, treating infections, or taking proper care of diseases like diabetes or kidney illness may all be included in this. Medication: Medication may occasionally be administered to treat a particular cause of blood volume loss or to stabilise blood pressure. For instance, drugs that encourage clotting or reduce bleeding may be given if bleeding is the root cause of the problem. Human albumin is the active ingredient of the 100ml human albumin 20% injection (Grifols). It comprises a human plasma-derived liquid albumin solution. It is given to patients to replenish blood or bodily fluids lost due to ailments such as heavy bleeding, surgery, or renal dialysis. Red blood cell replacement and oxygen-carrying capability restoration may be achieved with blood transfusions in cases of extreme blood loss. Monitoring and supportive care: Blood pressure, heart rate, and urine output must all be closely monitored in patients with hypovolemia. Supportive care may be given, such as oxygen therapy or pain control. It is crucial to remember that a person's health and needs should dictate how qualified medical experts deliver the treatment for blood volume loss. It is advisable to get immediate medical help if you or someone you know exhibits hypovolemic symptoms.  All ages are affected by the chronic lung illness known as asthma. Breathing becomes more difficult as a result of inflammation and muscular stiffness around the airways. Coughing, wheezing, shortness of breath, and chest tightness are among the symptoms. These signs and symptoms might be minor or major, and they can change over time. Inhalers are an important component of asthma management, and they can help prevent asthma attacks when used correctly. Here are some tips on how to use inhalers effectively to prevent asthma attacks: Understand Your Inhaler: There are different types of inhalers, including metered-dose inhalers (MDIs) and dry powder inhalers (DPIs). Each type has specific instructions for use, so it's essential to read the patient leaflet or receive proper training from your healthcare provider on how to use your specific inhaler correctly. Controller medications are taken daily to maintain asthma control and prevent attacks. They help reduce airway inflammation and keep symptoms at bay. Common examples include:
Follow the Prescribed Dosage: Use your inhaler as prescribed by your healthcare provider. It's important not to exceed or skip doses unless instructed otherwise. If you have any concerns about the dosage or frequency, consult your healthcare provider. Use a Spacer Device: A spacer is a chamber that attaches to the inhaler and helps ensure that the medication reaches your lungs effectively. It also reduces the risk of side effects, such as oral thrush. If your inhaler requires a spacer, make sure to use it according to the instructions. Proper Inhalation Technique:
Keep Your Inhaler Clean: Regularly clean your inhaler as instructed by the manufacturer to ensure proper functioning. A clean inhaler helps deliver the correct dosage and reduces the risk of contamination. Carry Your Inhaler: Keep your inhaler with you at all times, especially when you're away from home. This allows you to have immediate access to medication in case of an asthma attack or sudden symptoms. Regular Follow-Up: Schedule regular check-ups with your healthcare provider to assess your asthma control, adjust your medication if needed, and ensure that your inhaler technique is correct. Remember, while inhalers are effective in preventing asthma attacks, they are part of a comprehensive asthma management plan. It's important to work closely with your healthcare provider to develop a personalized plan that addresses your specific needs and includes other preventive measures, such as avoiding triggers and managing allergies, to minimize the risk of asthma attacks. Impetigo is an extremely contagious bacterial skin infection that predominantly impacts infants and young children, although it can also occur in adults, especially those with compromised immune systems. The primary culprits behind impetigo are typically the bacteria Staphylococcus aureus and Streptococcus pyogenes.
Treatment methods for impetigo typically involve a combination of antibiotics and good hygiene practices. To effectively get rid of impetigo, it’s important to follow a comprehensive treatment approach. Here are some steps you can take:
Interleukin (IL) inhibitors play a crucial role in the treatment of plaque psoriasis, a chronic autoimmune skin condition. Plaque psoriasis is characterised by the development of thick, red, and scaly patches on the skin, often accompanied by itching, discomfort, and a significant impact on quality of life. IL inhibitors specifically target and modulate the activity of certain interleukins, which are signalling proteins involved in the immune response and inflammation. Here are the key importance and uses of IL inhibitors in plaque psoriasis treatment:
|
Details
AuthorMrMed - India's most preferred online super speciality pharmacy. Get up to 85% off on Genuine Medicines at your Doorstep. 📞 89391 69999 Write something about yourself. No need to be fancy, just an overview. Archives
October 2023
Categories |






 RSS Feed
RSS Feed
